Published by: Maria Bryndina on 20.June.2022
White coat hypertension: worse than it seems to be. Critique
The phenomenon of “white coat” hypertension appeared with the first blood pressure monitor, before both white coats and the concept of hypertension appeared. It evolved from a test for fear of doctors to a harbinger of serious harm to health. However, there is no generally accepted definition and clear algorithms of actions when detected.
An Italian doctor Scipione Riva-Rocci, having invented the sphygmomanometer in 1887 and undertaken to test it, supposed that some of the experimental subjects had an increase in blood pressure due to its measurement1. However, at that time there was one and only Riva-Rocci apparatus on the planet and its one and only confident user, so there was no chance to check the guess on an outpatient basis. A little later, Nikolai Korotkov discovered systolic and diastolic blood pressure (BP), and in the second half of the 20th century hypertension was recognized as a dangerous disease requiring therapy2. Blood pressure monitors gradually became a part of a routine check-up, and then a popular household appliance. The term “white coat hypertension” was invented by practitioners, migrated from there to scientific literature along with interest in this phenomenon in the 1980s, and became generally accepted3-5.
White coat hypertension (GBH) is a phenomenon of increased blood pressure when it is being measured by a medical worker and / or in a medical institution alongside normal levels obtained during 24-hour (ABPM) or self-measured blood pressure monitoring4, 5.
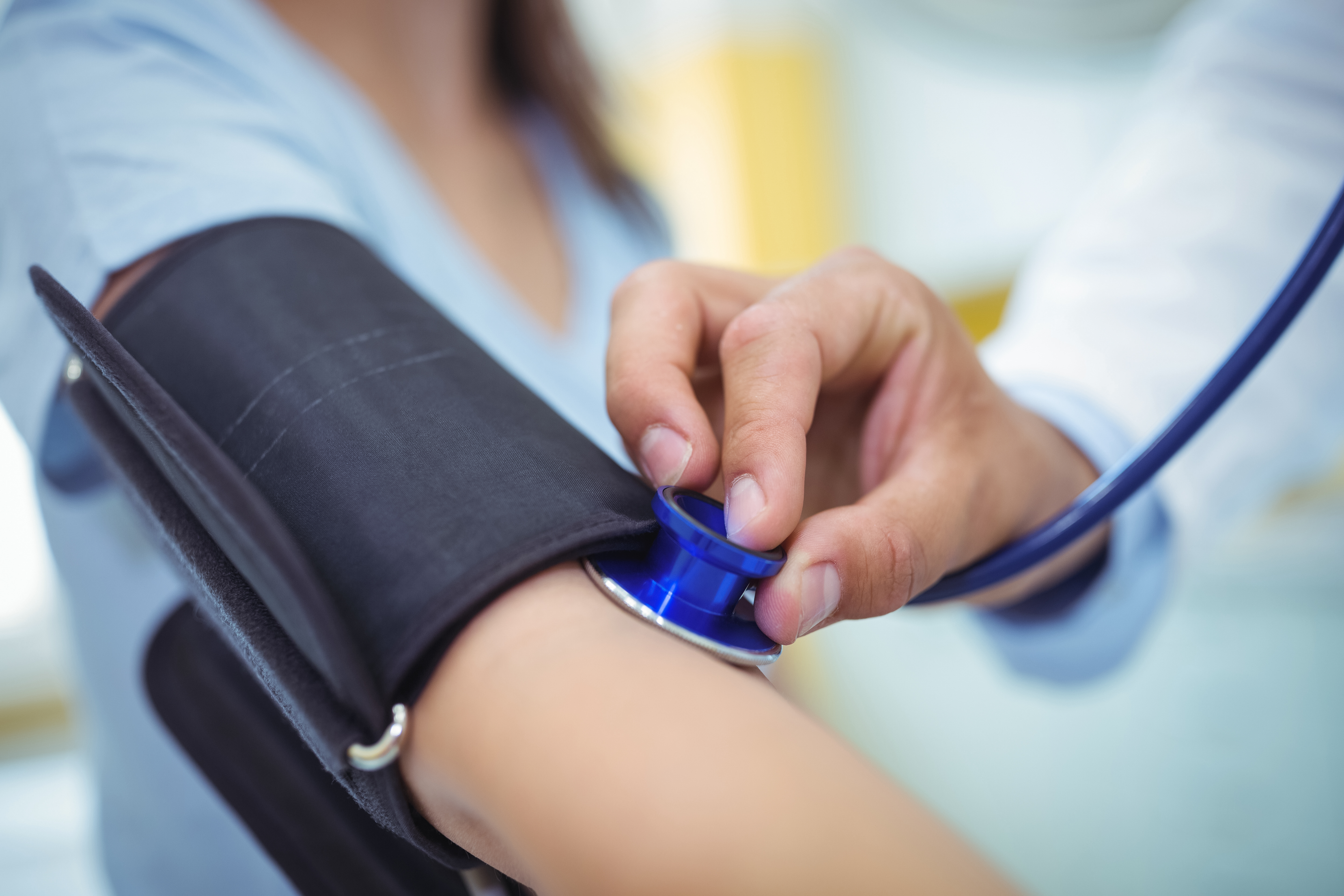
The European Society of Hypertension (ESH) relates the concept of GBH to apparently healthy people not receiving antihypertensive therapy. An increase in blood pressure under similar conditions in hypertensive patients already taking drugs, that are effective when a doctor with a tonometer is away, is proposed to be called the "white coat effect", combining both conditions into the "white coat syndrome" 4–6.
A state, that is the reverse of HCH, is distinguished as “hidden” or “masked” hypertension (masked hypertension) - normal blood pressure is recorded in a hypertensive patient, who does not receive antihypertensive therapy, during an examination by a doctor.
HBC Criteria
Whereas, cardiologists of the world are not of one mind on the HCH criteria (as well as on the degrees of hypertension in general). According to ESH, one can speak of a “to a white coat” reaction if the blood pressure at the appoinment is ≥140/90 mm Hg, and the average daily value is <130/80 mm Hg. (according to SMAD). The National Institute for Health and Care Excellence (NICE) raises the acceptable level of the average "home" pressure to 135/85 mm Hg. American College of Cardiology/American Heart Association, ACC/AHA is the strictest, as it draws a border of 130/80 mm Hg: if it is higher at the appointment, and lower at home (with ABPM or self-control), then there is HCH4.
A weak spot in the diagnosis of the "white coat" effect is the measurement of blood pressure in the "out-of-hospital" conditions, whether it is the patient's self-monitoring or ABPM. The patient may sincerely not be able to use the tonometer, or may deliberately lie. There is more faith in daily monitoring, but there is a room for the patient's creativity even there, it is enough to keep a self-control diary carelessly.
Due to the variety of criteria and the need to take self-reported data for granted, it is extremely difficult to estimate "white coat syndrome" morbidity; in different studies, from 10 to 50% of participants reacted with a significant increase in blood pressure to its measurement in a medical institution; according to the only meta-analysis, such people among hypertensive and (so far) healthy individuals are about 13%. In a large study of more than 115,000 people, about 35% of untreated participants met the "European" (ESH) criteria for HCH4.
Causes and risk factors
The causes of HCH are clear. Doctors, medical institutions and medical procedures are always stressful, even if you are not stabbed with sharp objects. The body responds to these troubles with moderate activation of the sympathetic nervous system and the secretion of stress hormones, and in most normal people, a small (within 10/5 mm Hg.) rise in blood pressure one is observed at the doctor's office, which does not go beyond the norm and daily fluctuations7. Anyway, a doctor with a tonometer is not as terrible as with a syringe. Doctors (with higher education), it must be mentioned, are more ‘scary’: when measured by nurses, blood pressure jumps were lower than when a doctor took up. The white coat has nothing to do with it either: predisposed patients have the same reaction to people in casual clothes (in a doctor's office) putting on a cuff4, 7, 8.
A significant increase in blood pressure when measured in the clinic often indicates a higher level of anxiety in this patient. For instance, such people react to the need for public speaking in a similar way. Moreover, HBC was relatively more often detected in men, older people who are obese and have increased levels of lipids in the circulating blood4. Obviously, these factors matter in “common” hypertension (AH), and excessive anxiety is not good for the body. Patients with white-coat hypertension showed a higher heart rate and no decrease in blood pressure at night (normally, a decrease by ≥10%), which indicates hyperactivity of the sympathetic nervous system. The relation between “white coat” effect and the indices of arterial wall stiffness was also shown in such patients 6. Thus, if the body reacts violently to a not too serious stimulus and/or walls - then this is not such a harmless state.
.jpg)
Consequences
People diagnosed with HCH are about 2.5 times more likely to develop HD 4 in the next 10 years 4. According to a recent small study (101 children, median age 14 years) the prognosis may be worse in children and adolescents: about a half of children with HCH may develop essential hypertension within a year9.
Currently, cardiologists are inclined to believe that HCH is something like a "pre-hypertension" stage, and if you "catch" it, then ... it's not clear enough what to do. Frankly speaking, there is nothing to treat. In two studies involving people with HCH over 60 and 80 years, "preventive" antihypertensive therapy resulted in a reduction in the risk of cardiovascular events, but these data cannot be extrapolated to a younger population4.
However, HCH should not be ignored: the risk of target organ damage and overall mortality in people with HCH without therapy in the next 3-19 years is significantly higher than in healthy ones and hypertensive patients with the "white coat" effect, who are already receiving therapy6, 10.
Doctors are busy apart from "pre-hypertension" patients, who may not progress. The only solution is after discounting essential hypertension (ideally by ABPM) to try to increasingly encourage people with HCH to periodically monitor their own blood pressure.
What about latent hypertension?
Latent / "masked" hypertension is equally dangerous. According to some data, up to 16% of the population can leave with elevated blood pressure, reducing it to normal values at rest when measured and, accordingly, without receiving antihypertensive therapy. These are, as a rule, young people with risk factors (heredity, obesity, diabetes mellitus), and the lack of treatment can result in bad consequences. This is confirmed by the data of meta-analyzes: the risk of developing cardiovascular events and associated mortality in latent hypertension is significantly higher than in diagnosed and treated hypertensive patients6, 11.
Those with the white coat effect who are already taking medications are the safest. Antihypertensive therapy enhancement is the worst consequence, so their cardiovascular risks do not differ from “ordinary” hypertensive patients and are significantly lower compared to people with HCH and especially latent hypertension4, 6.
As well as any non-standard situations, identifying and treating patients with HCH and latent hypertension, though it looks simple, requires time, money, and a medical worker involvement. However, in this case, the patient themself is mainly responsible for their health, and it is important, although very difficult, to communicate it to them.
References:
1. Mancia G, Parati G. Clinical significance of "white coat" hypertension. Hypertension. 1990;16(6):624-6.
2. Saklayen MG, Deshpande NV. Timeline of History of Hypertension Treatment. Front Cardiovasc Med. 2016;3:3.
3. Pickering TG, James GD, Boddie C, et al. How common is white coat hypertension? JAMA. 1988;259(2):225-8.
4. Nuredini G, Saunders A, Rajkumar C, Okorie M. Current status of white coat hypertension: where are we? Ther Adv Cardiovasc Dis. 2020;14:1753944720931637.
5. Parati G, Bilo G, Mancia G. White Coat Effect and White Coat Hypertension: What Do They Mean? Medscape. 2003.
6. Pioli MR, Ritter AM, de Faria AP, Modolo R. White coat syndrome and its variations: differences and clinical impact. Integr Blood Press Control. 2018;11:73-79.
7. Bloomfield DA, Park A. Decoding white coat hypertension. World J Clin Cases. 2017;5(3):82-92.
8. Clark CE, Horvath IA, Taylor RS, Campbell JL. Doctors record higher blood pressures than nurses: systematic review and meta-analysis. Br J Gen Pract. 2014;64(621):e223-32.
9. Brooks M. White Coat Hypertension May Progress to Hypertension in Kids. Medscape. 2020.
10. Cohen JB, Lotito MJ, Trivedi UK, et al. Cardiovascular Events and Mortality in White Coat Hypertension: A Systematic Review and Meta-analysis. Ann Intern Med. 2019;170(12):853-862.
11. Kjeldsen SE, Os I. Poor reproducibility of masked and white coat uncontrolled hypertension: important new information on MUCH and WUCH. Eur Heart J. 2020;41(16):1572-1574.
Colleagues, haven't you joined our PharmaCourses of MENA region Telegram chats yet?
In the chats of more than 6,000 participants, you can always discuss breaking news and difficult situations in a pharmacy or clinic with your colleagues. Places in the chats are limited, hurry up to get there.
Telegram chat for pharmacists of MENA region: https://t.me/joinchat/V1F38sTkrGnz8qHe
Telegram chat fo physicians of MENA region: https://t.me/joinchat/v_RlWGJw7LBhNGY0